- Denials Management Services
- A/R Follow Up Services
- Cash Flow Management
Our denial management services are customized according to the client’s practice needs and its revenue cycle requirements, with a constant focus on optimizing the practice’s cash flow.
Fact: Only 70% of the average healthcare practice’s insurance claims are ever paid by insurance providers. While a practice may submit a perfectly clean claim to a payer, there is no guarantee that it will be paid accurately, if it is paid at all.
It’s no secret that payers continue to impose increasingly complex rules, systems, and loopholes with the single goal of limiting payment. This frequently means that practices do not receive full payment for the valuable services they provide to their patients.
D Prince Management A/R Follow Up services constantly strive to upgrade its system to the most appropriate and latest tools and focuses on maximizing technology-driven automation of processes and report generation. This results in maximum efficiency and accuracy with minimal costs and allows the billing company to evaluate its performance using our powerful predicted revenue collection metrics, resulting in increased cash flow for the organization.

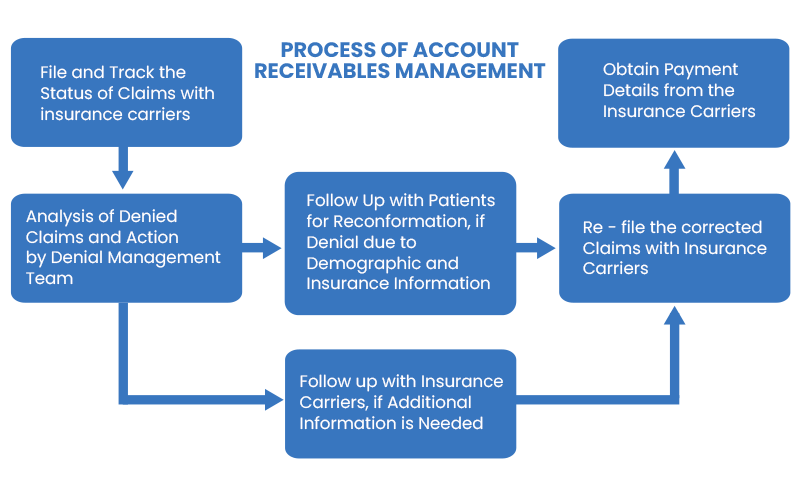

- Our staff is well-trained to work offline using spreadsheets, delivered reports or reports accessed and generated directly from the client’s software.
- Our accounts receivable (A/R Follow Up Services) professionals are experts in handling various insurance categories/plans, such as HMOs, PPOs, commercial insurers, workers’ compensation, Medicare, Medicaid, etc.
- To promote understanding and efficient issue resolution, our analysis and reporting system provides an in-depth breakdown of any issues that may arise, and our client relations team responds rapidly with recommendations on how to resolve issues and decrease A/R days outstanding and improve collections.
Cash flow management is one of the greatest challenges faced by healthcare organizations.
- We currently support various medical billing software packages
- We have experience handling billing for different specialties.
- Institution of an effective insurance verification system
- Initiation of comprehensive improvement of coding adherence to LMRPs and CCI
- Deep and comprehensive understanding of reimbursement contracts
- Deep and comprehensive understanding of payer procedures
- Robust tools and procedures for analysis of denials

